Recent studies show that over a 9 year period, infusion mix-up errors were the most common (22.6%; n = 205), of which 92% involved high alert drugs (e.g., heparin, insulin).
Current strategies to reduce infusion mix-ups are limited, with infusion setups varying between clinicians, units, and hospitals. Although interventions have been proposed, they have not been empirically evaluated except for a study that demonstrated infusion labels improved timely infusion identification. To this end, as part of a larger study they evaluated the impact of three interventions on the accuracy and speed of infusion identification and disconnection.
The study looked at materials and methods which included design, location/apparatus, conditions, procedure, metrics and analysis. The results suggest that line labels/organizers may increase infusion identification, accuracy and efficiency, yet there is no standard practice regarding their use currently in the ICU.
You can be the hero that finds an easy to use and very cost effective solution while being compliant and significantly reducing errors and potential harm to patients. To hear more on how we can customize this solution for your ICU or other departments, you can contact us at (800) 206-9147.
The Solution:


Benefits:
1) Labels are big and bold which is easier for nurses to read in the low light environment of ICU.
2) All labels are created on demand and in a clean and enclosed housing which reduces infection risk.
3) No handwriting required so 100% legible all the time.
4) No guesswork concerning standards on when to change tubing.
To read the full study and find additional information please click on the link below:
The Importance of Labeling Intravenous Tubing
See It Work Here:

Simex Subglottic Aspiration Device
Only FDA cleared Subglottic Aspiration Device. Guarantee to pull out more secreations then wall suction. Reduce infection and reduce cost.
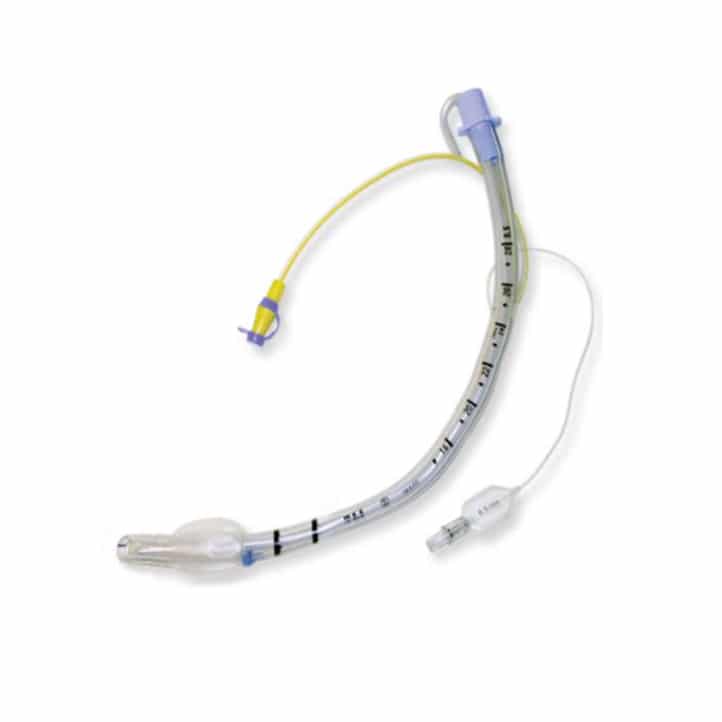
NeVap ET tube w/ Subglottic Port
Recent News and Insights

Attention: Important Information For Clinicians Treating Coronavirus Patients On Mechanical Ventilator.
Resources to Stay Informed:
NIH.gov
Covid Articles


